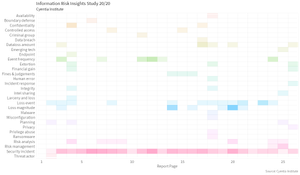
The Cyentia Library Relaunches
I'm excited to see that they're Re-introducing the Cyentia Research Library, with cool (new?) features like an RSS feed. There are over 1,000 corporate research reports with data that companies paid to collect, massage, and release in a way they felt would be helpful to the rest of the world.


